Liz Calise remembers the morning in 2009 she woke up and her world quite literally flipped. Her bedroom began spinning and she couldn’t keep her balance.
“That was the beginning of my nightmare,” she said. “The dizziness episodes kept happening over and over again.”
A visit to the ER and then to an ear, nose and throat doctor failed to provide answers. The doctor prescribed anti-nausea pills and dizziness suppressants, but the vertigo-like attacks kept occurring. Liz’s worsening health forced her to retire from her job as assistant manager at a supermarket deli in central Florida.
 Liz Calise poses with Dr. Samy Youssef after undergoing successful endoscopic brain surgery in Florida in 2013.
Liz Calise poses with Dr. Samy Youssef after undergoing successful endoscopic brain surgery in Florida in 2013.
Her husband, Andrew, said her condition deteriorated even more over Thanksgiving 2010. “She started acting strange. She was sort of out of it, like in a daze,” he said. “She woke up one day and had no strength to keep her body up. She was like dead weight.”
Discovering Dr. Youssef
He took her to a neurologist who did some research but couldn’t find anything. “I said, ‘Look at my wife, she’s like a zombie,’ and she was getting worse.”
The next neurologist they visited diagnosed Liz with hydrocephalus – fluid on the brain – which was caused by a large cyst deep inside her brain. However, he said, surgery would be too risky. In all, the Calises consulted with seven neurologists and neurosurgeons and always heard the same thing: too risky.
Just as the couple, who have three sons and three grandchildren, were running out of hope, they went to see Mark Shaya, MD, a neurosurgeon in Miami. He told them he’d just been to a Florida Neurological Society meeting where he’d heard a presentation by Samy Youssef, MD, PhD, then an associate professor at the University of South Florida in Tampa Bay.
Youssef, who in 2014 joined the University of Colorado School of Medicine’s Department of Neurosurgery as a professor of neurosurgery, gave a talk about endoscopic, minimally invasive brain surgery techniques, which have grown in sophistication over the last 20 years.
Brain surgery revolutionized
“Brain surgery has been revolutionized by advances in technology – namely imaging technology, advanced microscopes and endoscopes, and navigation tools,” Youssef said. “It has made brain surgery, even for complex brain tumors, much more precise and much less invasive, with faster recoveries and shorter hospital stays for the patients.”
The Calises were ecstatic to learn about Youssef and his expertise with endoscopic techniques and minimally invasive brain surgery. Liz, at the time in a wheelchair and losing cognition, got an immediate appointment.
Youssef discovered that Liz’s condition is very rare. The large cyst growing out of her thalamus, a veritable “grand central station” structure that sends neurologic information to the rest of the body, was obstructing the flow of cerebrospinal fluid and causing pressure to her brain. “It’s near the pineal structure of the brain,” he said. “It’s deep in the brain and around critical blood vessels on the back of the brain stem. Surgery there is challenging.”
Researching this rare condition
In a study recently published in World Neurosurgery, Youssef and five other researchers, including CU Anschutz Neurosurgical Fellow Ciro Vasquez, MD, wrote that medical literature has reported only 13 cases in which a cyst originated in the thalamus and involved the brain’s third ventricle – a cavity through which cerebrospinal fluid travels. He had previously performed endoscopic surgery to remove tumors and lesions in the pineal region, but not to reach a cerebrospinal fluid cyst in that area.
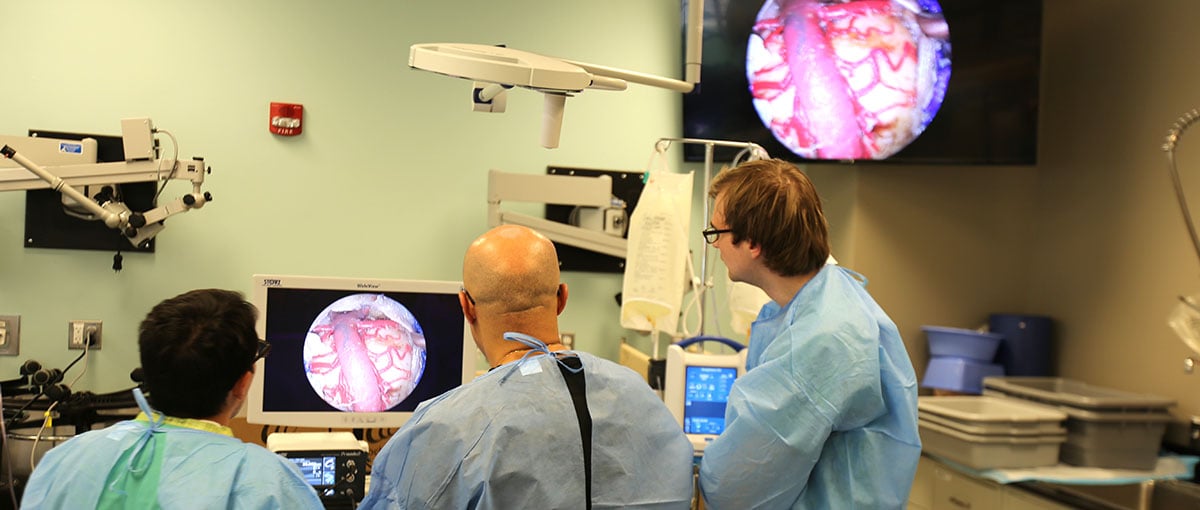 Samy Youssef, MD, PhD, professor of neurosurgery in the CU School of Medicine, (center) teaches two neurosurgeons on a minimally invasive brain surgery using live imaging technology in the Center for Surgical Innovation.
Samy Youssef, MD, PhD, professor of neurosurgery in the CU School of Medicine, (center) teaches two neurosurgeons on a minimally invasive brain surgery using live imaging technology in the Center for Surgical Innovation.
In Liz’s case, Youssef deployed similar technology, but used a different trajectory to reach the cyst, which he believes was an anomaly Liz was born with and worsened over time. If left untreated, her condition would have continued to deteriorate, likely leading to a dementia-like state. Youssef used a navigating endoscope with a special trajectory that reaches all the way through the ventricular system and into the deep-seated third ventricle. The entry point is a “keyhole,” or a single burr hole, behind the hairline on top of the skull.
Like ‘Fantastic Voyage’
“It’s like the movie ‘Fantastic Voyage’ – often times I show that footage in my lectures. It’s how fiction becomes reality,” Youssef said. “We’re navigating inside the human brain without opening it much.”
[cucalloutbox align="right" color="" class="" size=""]
Center for Surgical Innovation
Samy Youssef, MD, professor of neurosurgery, said that in addition to the specialized expertise available from the Complex Cranial and Skull Base Surgery program at the CU Anschutz Medical Campus, the campus benefits from having the Center for Surgical Innovation (CSI). His research focuses on complex brain surgery and minimally invasive techniques, and “having the CSI lab is a great resource to maintain that academic field of the skull base surgery,” he said. “We refine surgical approaches that get transferred from idea to lab, and from the lab to the operating room.”
Also, the Department of Neurosurgery offers a Skull Base Surgery year-long fellowship/resident program that uses the CSI Microsurgery Laboratory to give young neurosurgeons exposure to complex cranial cases and minimally invasive skull base approaches. This year’s fellow, Ciro Vasquez, MD, co-authored with Youssef the recent study, “Third Ventricular Cerebrospinal Fluid Cysts of Thalamic Origin,” published in World Neurosurgery.
[/cucalloutbox]
In a surgical procedure that only took an hour, Youssef used an endoscope to open and drain the cyst to the normal cerebrospinal fluid circulation. He then performed a ventriculostomy – a diversion of spinal fluid into the extra-ventricular cerebrospinal fluid system. “It uses the endoscope to create a natural passage for fluid to drain through a different channel to the rest of the spinal fluid drainage system,” he said. “So, it was two procedures in one.”
Within 24 hours of surgery, Liz’s cyst was significantly smaller, and within 72 hours she was responding to the post-op therapy. Her life was restored.
‘Back to myself again’
“I just woke up and was back to myself again,” Liz, 66, recalled of the surgery in 2013. “I could talk to my children, I had all my faculties, and I wasn’t shaking anymore. It was a miracle, just totally a miracle.”
Typically, a patient who undergoes brain surgery for a longstanding problem would go directly to a rehabilitation facility from the hospital. That wasn’t the case for Liz. She was able to go home. “Her speech came back completely; it was like she never had the problem before,” Andrew said. “She was the talk of the ward.”
Youssef has since performed two more endoscopic procedures on cerebrospinal fluid cysts of thalamic origin – both at University of Colorado Hospital – with similar success. The patients’ conditions were similar to Liz, and like her, they struggled to find a neurosurgeon willing to perform surgery.
“The amazing part of this disease entity,” Youssef said, “is that somebody’s life can be completely restored through a one-hour surgery and a single keyhole.”
‘On the map internationally’
Youssef, who travels the world teaching endoscopic, minimally invasive brain surgery procedures, was recruited by Department of Neurosurgery Chair Kevin Lillehei, MD, to direct the Complex Cranial and Skull Base Surgery program at CU Anschutz. The program, which is unique in the Rocky Mountain region, includes co-directors Samuel Gubbels, MD, and Vijay Ramakrishnan, MD, both associate professors of otolaryngology. “Now the program is on the map nationally and internationally,” Youssef said.
These sophisticated procedures are among the most challenging in neurosurgery, he said, but the results are life-changing. The average endoscopic brain surgery patient goes home after three days in the hospital, Youssef said.
“There is not much room for error,” he said. “We chose this field and we do these cases because of that reward we get at the end of the day when we see these patients go back to their normal lives, their families, their businesses. Everyone is happy. That’s what keeps us going in this field.”
The Calises, meanwhile, are back to enjoying their retirement years in the Sunshine State. They keep in touch with the neurosurgeon who changed their lives. “Out of all the doctors, he gave us light at the end of the tunnel,” Andrew said. “He drew a diagram of what he could do to help, and then he did it. Dr. Youssef is absolutely amazing.”




