For more than two decades, Jim Walsh’s heart has been an uncertain ally.
Like all of us, Walsh, 67, relies on that vital muscle to keep blood pumping to his body. But his can’t do the job alone. Late last year, damage to Walsh’s heart that began more than two decades earlier caught up with him. Two days before Christmas, Walsh lay on an operating table at UCHealth University of Colorado Hospital for a procedure to lend his failing heart a helping hand.
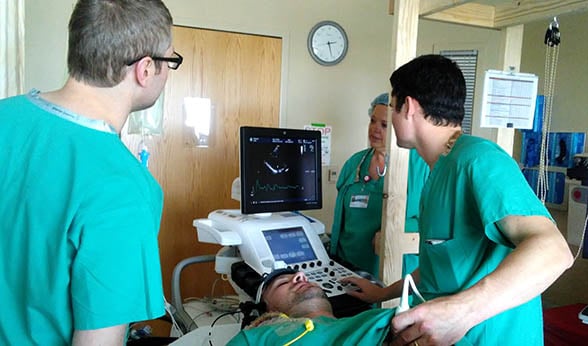 William Cornwell, right, performs an echocardiogram on volunteer Scott Ferguson in a CTRC lab as research coordinator Greg Coe looks on. It's part of Cornwell's five-year NIH-funded study aimed at better understanding the physiological effects of LVADs.
William Cornwell, right, performs an echocardiogram on volunteer Scott Ferguson in a CTRC lab as research coordinator Greg Coe looks on. It's part of Cornwell's five-year NIH-funded study aimed at better understanding the physiological effects of LVADs.
Cardiac surgeon Joseph Cleveland, MD, implanted a left ventricular assist device (LVAD) called the Heartmate 3, a pump designed to give Walsh’s weakened heart a big boost. Cleveland and his team hoped the LVAD would, in turn, lessen the pressure on Walsh’s pulmonary artery and right ventricle, which are responsible for supplying blood to the lungs for oxygenation.
The procedure happened none too soon. “My progression downward was rapid,” Walsh said. “I had the choice to die rapidly or get an LVAD.”
Long road
Walsh’s lengthy battle with congestive heart failure began in 1995 when tests revealed that the left main stem of his coronary artery had developed an aneurysm – a bulge that weakens the vessel wall and puts it at risk of rupturing. The finding surprised Walsh, who was then a relatively young man who had forged a successful career as an expert in finance for several major companies. He described himself as “asymptomatic” up to that point and added that he regularly jogged and lifted weights.
But the aneurysm worsened and required a surgical graft repair. A London surgeon used a section of Walsh’s mammary artery to bypass the aneurysm, but during recovery the graft failed and Walsh suffered a heart attack. A second graft, using a piece of saphenous vein in his leg, “held true,” but over the next decade his exercise capacity declined steadily, and he required ever-increasing doses of medications, such as diuretics, to manage his condition.
The problem continued to worsen as the years wore on. When he began treatment at the Denver VA Medical Center in 2014, Walsh’s advanced heart failure dangerously increased the pressure on his pulmonary artery. He was admitted to UCH in November 2016 under the care of CU School of Medicine heart failure specialist William Cornwell, MD. Andreas Brieke, MD, medical director of the Mechanical Circulatory Support Program for CU, also contributed to the case. Considered too great a risk for a transplant, Walsh chose the LVAD implant a month later.
 Jim Walsh is feeling stronger after receiving an LVAD just before Christmas last year. But he's still working to recover his stamina, even with the help of the pump. Photo courtesy of Jim Walsh.
Jim Walsh is feeling stronger after receiving an LVAD just before Christmas last year. But he's still working to recover his stamina, even with the help of the pump. Photo courtesy of Jim Walsh.
The surgery was successful, and Walsh is making a slow recovery that he hopes will one day lead to a heart transplant. He makes regular walks around Sloan’s Lake in northwest Denver – about 2.5 miles.
But Walsh’s case points to a larger question about the device that saved his life. Interviewed four months after the LVAD surgery, he said the lake walk still leaves him breathless, especially if he tries to talk at the same time.
The problem of the pump
Why hasn’t the LVAD pump been able to restore Walsh’s ability to normally complete this routine activity? That’s a question that intrigues Cornwell and his colleagues at CU. Cornwell is exploring it with the help of a five-year National Institutes of Health grant that began late last year. He’s equipped a lab in the Clinical and Translational Research Center (CTRC) on the 12th floor of UCH’s Anschutz Inpatient Pavilion to measure exercise capacity in patients with normal hearts, those with mild heart failure and those with LVADs. The work includes frequent measures of patients’ blood pressure, cardiac output, blood flow from the heart to the brain, blood oxygen levels and more while at rest and during exercise.
Cornwell notes that while LVADs are designed to pump 4 to 10 liters of blood per minute to the body, tests show that many patients with the pumps continue to have muscle atrophy and difficulty exerting themselves without their blood pressure and heart rate rising rapidly and fatigue setting in. These are all signs that the pumps might not be delivering a sufficient blood supply to the body’s muscles and organs.
“Many LVAD patients remain functionally incapacitated,” Cornwell said, with low oxygen consumption rates and other clinical symptoms that belie many patients’ subjective reports of feeling better after getting the devices.
In addition, work by Cornwell’s colleague Amrut Ambardekar, MD, CU cardiovascular specialist and medical director of the Cardiac Transplant Program, shows that artery tissue in the hearts removed from transplanted LVAD patients is often stiff and scarred beyond what would be expected with normal aging.
Case of the missing pulse
The problem may lie in the fact that LVAD patients lose something that most of us take for granted: the pulse created by heart contractions. The LVAD’s mechanical pump supplies blood in a continuous flow.
That’s led to known problems. For example, LVAD patients are at higher risk of gastrointestinal bleeding and stroke. The recently approved Heartmate 3 attempted to address the no-pulse problem by regularly speeding up and slowing down the pump rotor – a kind of artificial heart “lub-dub.” But Cornwell said data thus far show that the feature has not decreased the rate of strokes or bleeding.
Losing the pulse has other “subtle but important implications,” Cornwell said. The heart’s contractions stretch a network of sensors in the aorta and carotid arteries called baroreceptors. These sensors communicate with the brain, helping to regulate blood pressure naturally. In LVAD patients, by contrast, the lack of a pulse “revs up” the sympathetic nervous system, which releases adrenaline and increases blood pressure, thus interfering with normal blood flow.
That may help to explain why many LVAD patients such as Walsh don’t see improvement in their capacity to walk at least short distances without fatigue, climb stairs or do regular household chores, Cornwell said. One question to be answered in the lab is whether LVADs can be made to sufficiently increase blood flow to the body during exercise to compensate for the absence of pulse.
Into the lab
Any conclusions await data gathering. Cornwell is now testing healthy patients. Those with mild heart failure and with LVADs will follow. On a recent afternoon, volunteer Scott Ferguson lay on a bed in Cornwell’s lab. An array of lines to measure cardiac output, heart and lung pressure, blood oxygen levels, and other data ran from Ferguson’s arm and neck. A transcranial device fitted around his head would measure the flow of blood to his brain. Cornwell also took an echocardiogram to get an image of Ferguson’s heart.
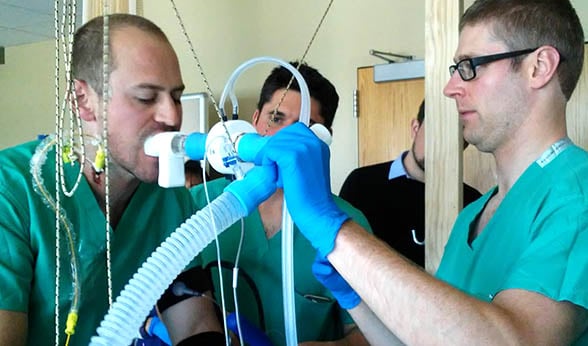 Research coordinator Greg Coe fits a breathing tube on volunteer Scott Ferguson while William Cornwell watches. Ferguson completed three stages of steadily demanding cycling to measure the physiological effects on his body.
Research coordinator Greg Coe fits a breathing tube on volunteer Scott Ferguson while William Cornwell watches. Ferguson completed three stages of steadily demanding cycling to measure the physiological effects on his body.
A team of CTRC nurses assisted with monitoring Ferguson and taking regular blood draws, which would later measure arterial blood gases during periods of rest and exertion. Greg Coe, clinical research coordinator and regulatory specialist at CU, stood before twin towers of computer monitors displaying many fields of colored lines running in peaks and valleys. These were the representations of Ferguson’s body at work: heart and respiration rate, blood pressure, pulmonary artery pressure and much more.
Ferguson, 29, a post-doctoral fellow in cardiovascular physiology at CU, lay calmly on the bed while Cornwell and his team readied him for the tests. Cornwell asked him to breathe in and breathe out, then to bear down for 20 seconds. Coe timed the exercise while monitoring the readings at the two screens.
With that completed, Ferguson stood and mounted a stationary bike. Coe inserted a long breathing tube in his mouth and clipped his nose. Over the next hour or so, he completed three regimens of timed cycling with low, moderate and intense levels of exertion. During each one, nurses drew blood while Ferguson pointed at a clipboard to silently indicate to Coe his level of exertion. Cornwell orchestrated the work while scrutinizing the lines on the computer screens that charted the changes in Ferguson’s physiological functions as he increased his exertions.
Steps ahead
It will be several months before an LVAD patient enters the CTRC lab to provide the same kind of data, Cornwell said. But the work with healthy patients and those with mild heart failure will provide useful comparisons when he and his team examine the responses to exercise of pulseless LVAD patients.
“We’d like to see how much exercise it takes to create a physical pulse using the heart’s natural power,” he said. That might lead to “novel exercise prescriptions,” such as lifting resistance weights or interval training.
“These devices [LVADs] are important, but it doesn’t mean that we stop working,” he said. “Patients improve with them, but they are not out of the woods.”
Walsh is grateful for the lifesaving care he received from the entire CU team at UCH and is ready to do whatever he can to help further. If he is eligible for a transplant, he’s willing to allow study of his damaged heart and said he “absolutely has the same enthusiasm” for Cornwell’s study.
The strongest drive lies close to home: his wife and three daughters, including the youngest, who is just 14 years old.
“My hope is to be here long enough to help her navigate her way through her formative years in high school and, perhaps, even university,” he said. “I’m not afraid of death, but I’d like to think that with the LVAD I have bought more time before the statistics turn against me.”




